Heated and humidified gases
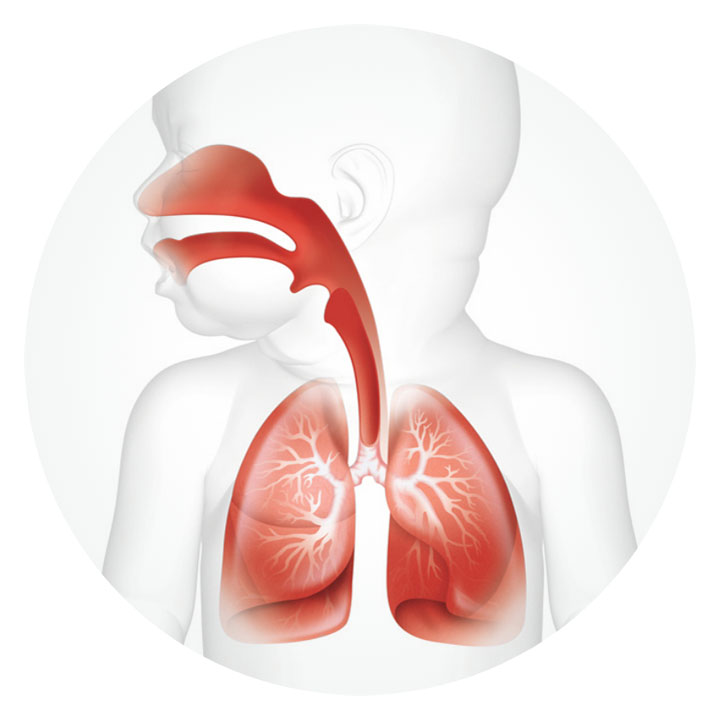
In a healthy airway, gas is heated and humidified by the upper airway during inspiration and fully saturated with water vapor at core body temperature (typically 37 °C, 44 mg/L H2O ) when it reaches the distal airways.1
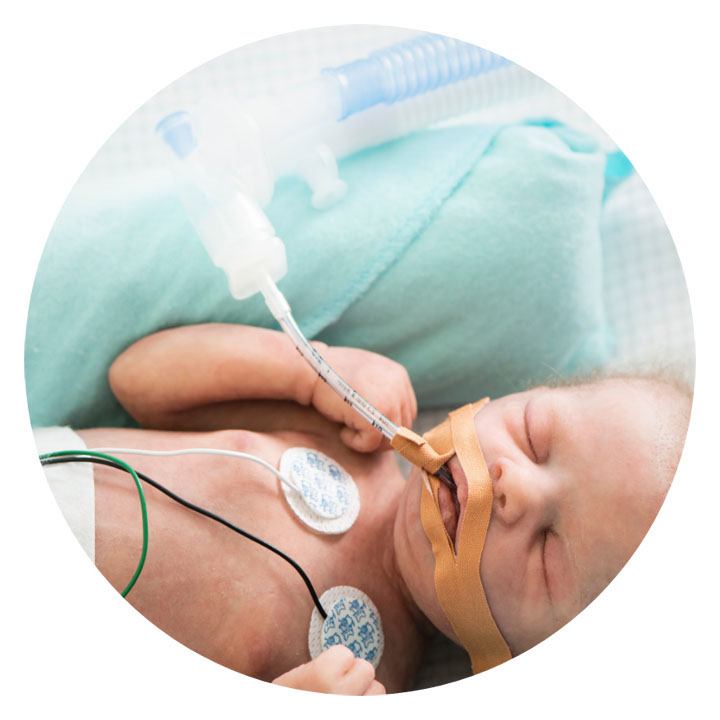
However, during invasive ventilation, the upper airway is bypassed, along with its natural airway protection and humidification mechanisms. Therefore, heating and humidifying gases while this treatment is being delivered is crucial.1,2
Why is humidification important?
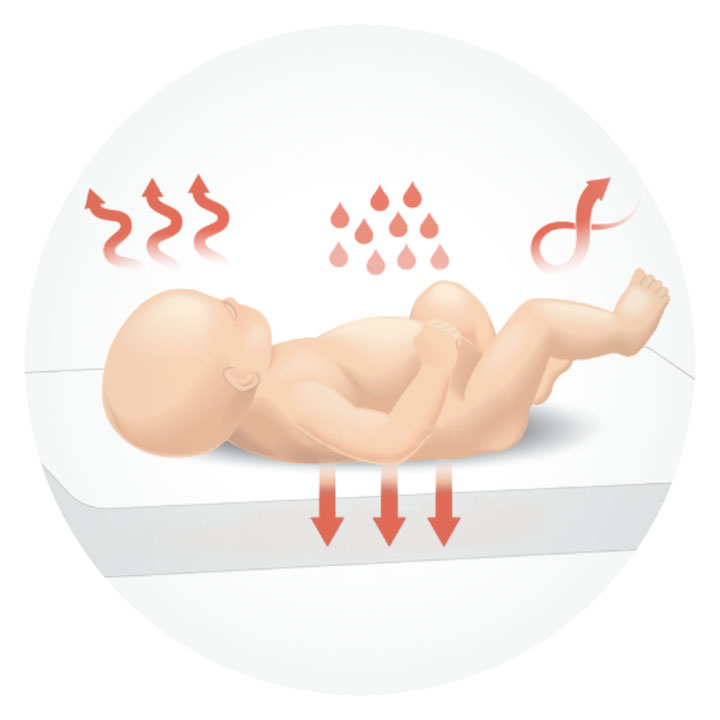
Medical gas is typically cold and dry (≤ 23°C, < 2% relative humidity) compared with ambient air (23 °C, 40% relative humidity).3 The delivery of cold, dry gas to the airway is associated with increased water and heat loss, inflammation in the airway epithelium, and an increased risk of airway injury. Insufficient humidification may also impair secretion clearance and increase the risk of airway blockages. These effects are amplified in preterm infants, where a few minutes of ventilation with insufficient humidification has been shown to increase airway resistance and reduce lung compliance.1,2
There are several key benefits associated with humidification.