A newborn’s respiratory system is reliant on humidity to maintain physiological balance, assist natural defense mechanisms, and conserve energy for growth and development.
The benefits of delivering heated and humidified gases during all forms of respiratory support is well recognized from research1–4 and clinical practice.5–7
What is humidity?
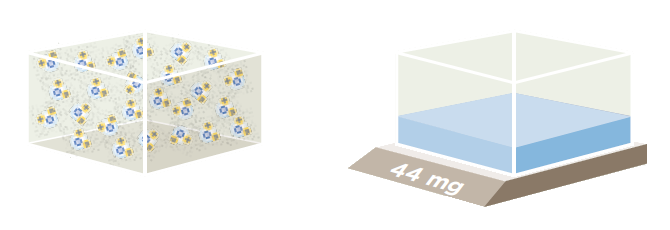
Absolute Humidity (AH)
This represents the total amount of water vapor in a given volume of gas in which it is contained. Absolute Humidity is measured as mass divided by volume of gas (mg/L).
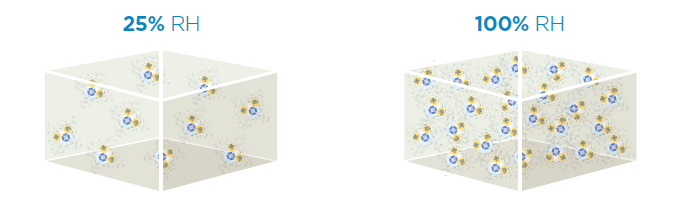
Relative Humidity (RH)
This takes into account the water contained in the gas, compared with how much water it can hold before the vapor condenses to liquid water. Relative Humidity is measured as a percentage
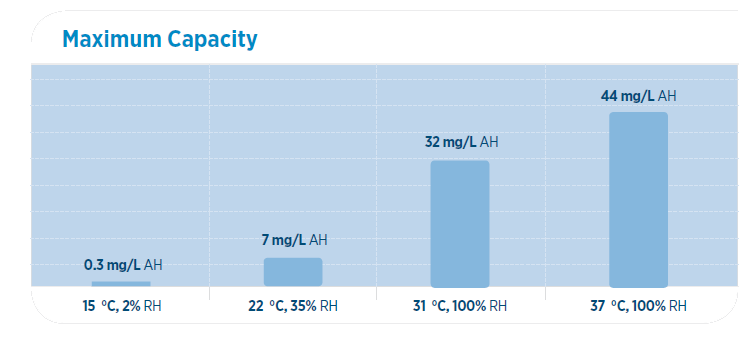
Temperature affects humidity
The quantity of water vapor that gas can hold increases with the temperature of the gas. A warm gas can hold more water vapor than a cold gas.3
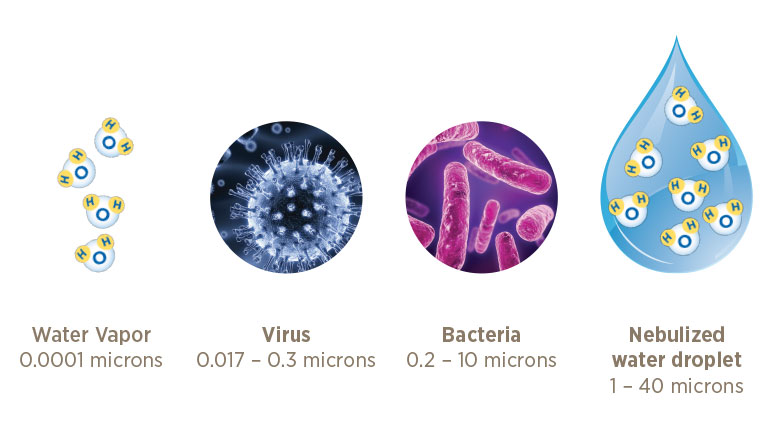
Particle size
Water vapor particles are too small to transport bacteria or viruses. Heated humidifiers generate water vapor.8–12
Why is humidification important?
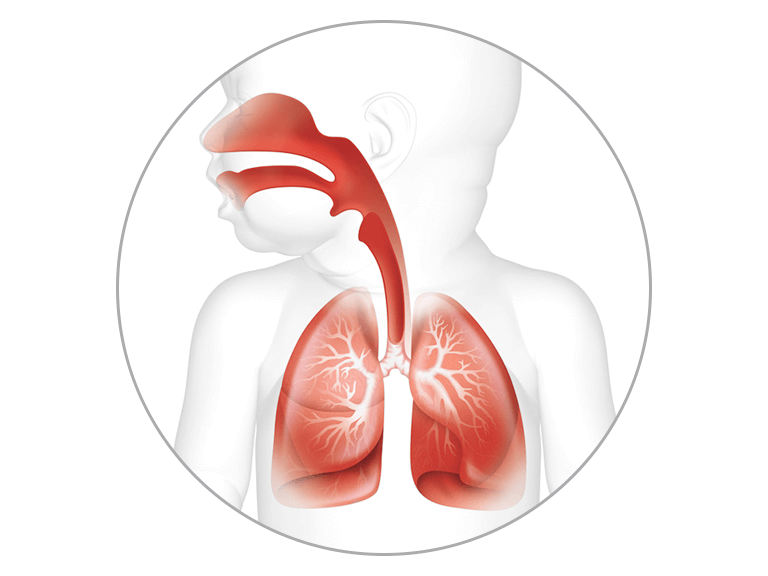
Assists natural defense mechanisms in the airway
The primary defense mechanism: Reflexes such as sneezing, coughing, and gagging are supported by the natural filtration of nasal hairs and the upper airway. In preterm infants, these mechanisms can be underdeveloped.13–15
Mucociliary transport – the second line of defense: The role of the mucociliary transport system is to trap inhaled contaminants (in mucus) and transport them up and out of the airway. The efficiency of this mechanism is reliant on several factors, including the temperature and humidity of inspired gas.16,17
The lower the humidity of the inspired gas, the further it needs to travel down the airway before physiological temperature and humidity are reached.18
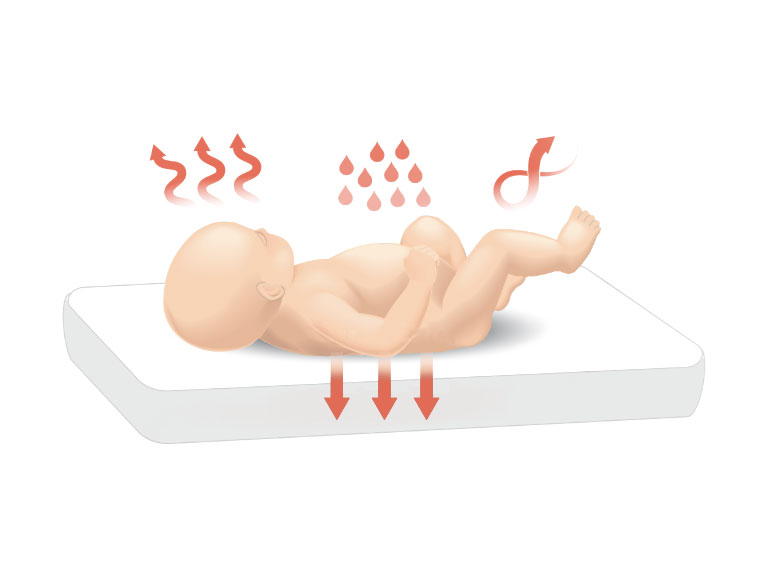
Promotes conservation of energy for growth and development
At birth, newborns are exposed to immediate cold stress and heat loss. Premature infants may also have limited heat production capabilities, along with an increased need to conserve limited energy reserves.19
Infants need energy for growth and development; therefore, assisting in thermoregulation is important. There is a range of interventions such as ensuring a neutral thermal environment, drying towels and blankets, a radiant warmer, or skin-to-skin contact.
Humidifying delivered therapies is also important to promote conservation of energy. When inadequate levels of humidity are inhaled, water vapor is drawn from the airway mucosa until the inspired gas has reached 37 °C, 44 mg/L. The energy cost to the infant for each gram of water removed from the mucosa is 0.58 kCal (2.4 kJ).20
Supports patient comfort and therapy tolerance
In addition to assisting natural defense mechanisms in the airway and promoting conservation of energy for growth and development, adequate humidification during respiratory support has been found to increase patient comfort and therapy tolerance.4,21–23
While this data is derived predominantly from adult patients, the principles are also applicable to pediatric population.24–26 In particular, humidification is associated with clearance of retained secretions and prevention of airway drying, which may subsequently improve lung compliance and work of breathing.27–29
